
Oregon Considers Changing The Way Mentally Ill People Are Committed
Listen
Last year, Don Baglien’s 19-year-old son experienced a psychotic break. It was a Sunday afternoon. He picked up the family picnic and threw it over the fence. Then he started turning on every faucet in the house, dragging furniture outside and howling.
“By the time the evening rolled around, he was convinced that his air conditioner unit had some kind of poison in it and was releasing some kind of toxic chemical that was going to kill him. So he unplugged it and he was going to roll it down the hill and get rid of it,” Baglien said.
It got so bad Baglien called the Roseburg police and had him arrested for menacing. Baglien worked with the local behavioral health provider to get him help. But since his son is an adult, he couldn’t intervene and things got worse.
“There were at least six or seven times when things were so out of hand that it was clear that he needed to get a bed somewhere where someone could keep an eye on him,” Baglien said.
Although the 19-year-old has been diagnosed with schizophrenia, he does not accept that he’s ill. Baglien has tried to get him civilly committed by having people argue in front of a judge that he’s a danger to himself and others – that’s the legal standard in Oregon.
But during those proceedings, his son understood enough to appear rational and calm – convincing the judge not to commit him.

Although Don Baglien’s 19-year-old son has been diagnosed with schizophrenia, he does not accept that he’s ill. Baglien has tried to get him civilly committed but his son understands enough to appear rational and calm in front of a judge. CREDIT: KRISTIAN FODEN-VENCIL/OPB
It happens a lot according to Josephine County Judge Pat Wolke.
“What we’re talking about are the people who will not get voluntary treatment. Because they have a condition called Anosognosia. And that means that they’re so ill that their ability to even understand that they’re ill has been taken away from them,” Wolke said.
Civil commitment is a delicate issue for families and authorities. The way it works now is that when someone threatens a family member or runs through traffic screaming at cars, police can place a hold on them. A county judge then decides whether they’re “a danger to self or others.”
But that legal standard has not been defined by the courts.
The process is justifiably difficult. But many think it’s become so difficult that people only end up getting help after they break the law and are criminally committed. So Oregon is thinking about changing the way people with mental illnesses are civilly committed.
Chris Bouneff lives with a mental illness and heads the Oregon branch of the National Alliance on Mental Illness. He understands the reluctance to civil commitment.
“Just because we have a mental illness and we’re symptomatic doesn’t mean we’re stupid or drooling on ourselves. I mean we have a sense of reality. We’re able to understand, if we’re before a judge, that I may lose my liberty,” Bouneff said.

Chris Bouneff lives with a mental health disorder and heads the Oregon branch of the National Alliance on Mental Illness. CREDIT: KRISTIAN FODEN-VENCIL
Civil commitments have been appealed so many times that the legal standard has gradually become harder and harder to meet. For example, one threat of suicide is no longer enough to prove a danger, according to the courts. And any perceived danger has to be “highly probable,” not just likely.
“We’ve reached a point where the bar is so high, that really the only way to enter the Oregon State Hospital, for example, is to be arrested. And we find that to be unacceptable,” Bouneff said.
He said Senate Bill 763 aims to decriminalize mental illness and is a minimal fix. The bill would define “dangerous to self or others” as “likely” to inflict serious harm within the next 30 days.
The bill also dictates that one threat of suicide can now be considered by a judge.
“We certainly don’t want to open the floodgates. We don’t want to make it so easy that we’re overusing civil commitment. But the bar has to come down a tiny bit because we are losing people,” Bouneff said.
But people in the mental health community are far from united in support of this bill.
Beckie Child was abused as a kid and suffers from PTSD. She’s also been held for civil commitment. She thinks the state should focus more on treating the early stages of mental illness instead of worrying about civil commitment.

Beckie Child was abused as a kid and suffers from PTSD. She’s also been held for civil commitment. She thinks the state should help people prevent mental health crises, rather than focusing on civil commitment.
CREDIT: KRISTIAN FODEN-VENCIL/OPB
“We do so little to keep people from getting into crisis. And then, when they are in crisis, then we decide we have to do all these other things that really can disrupt people’s lives and cause a lot of harm,” Child said.
Senate Bill 763 came out of a task force put together by Wolke. He hopes the bill will mean more people get help sooner, instead of descending into crisis and only getting help after they’ve been arrested.
He also thinks it’ll save the state a lot of money.
“We’re stopping people from repeatedly going to the emergency room. We’re stopping people from repeatedly getting arrested and going to jail,” Wolke said.
He was pleased last month when the Oregon Legislature Fiscal Office found that the cost of the measure was “indeterminate,” likely avoiding opposition based on cost.
But then, the Oregon Health Authority added its own fiscal statement, saying the agency may have to open a new unit at the Oregon State Hospital to look after all the new people who might be civilly committed.
The OHA estimated the cost at about $20 million over four years.
Wolke was frustrated because that figure only represents part of the financial equation.
“Yes, it will save the corrections department money. It will save hospitals money, it will save police departments money. But if it costs the Oregon Health Authority which did the fiscal impact statement, a little bit more money then they’re entitled to deep-six it with their fiscal impact statement – it’s just nuts,” Wolke said.
He wishes the departments that would save money under the bill would submit their own legislative impact statements.
The Oregon Department of Corrections agrees that if the bill becomes law, fewer people would likely end up in custody. But the department said it would be very difficult to calculate the exact savings.
Marion County Sheriff Jason Myers, who represents the Oregon State Sheriff’s Association, said the same is true for jails.
“I believe that lowering the bar would help certain individuals and it would help our local communities in terms of resources and freeing up resources,” Myers said.
Apart from which department might save what under this bill, there is another simmering argument. It revolves around where people with mental illnesses should receive treatment — at small community clinics, or at a large institution like the Oregon State Hospital.
Sarah Radcliff an attorney with Disability Rights Oregon, said the Oregon State Hospital is not the right place to spend it.
“To spend $20 million just in the next four years to expand the population at the Oregon State Hospital, those are dollars that are sorely needed in terms of community-based supports … longterm solutions like supportive housing and community mental health,” Radcliffe said.
Meanwhile, despite wide agreement, the civil commitment process is broken, but with questions surrounding the best ways to fix it, the bill sits in the Ways and Means Committee — unclear if it’ll ever make it to the Senate floor.
Copyright 2019 Oregon Public Broadcasting
Related Stories:
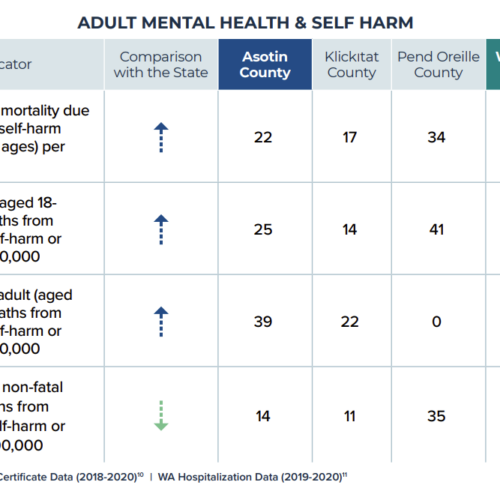
Asotin County assessment shows needs in mental health, housing, substance use treatment
An assessment by the Asotin County Health District shows that mental health, housing and aging in place, along with substance use, are some of the largest health issues facing the community.

Rape, beatings and racial slurs: None of it was enough to shut down this Idaho youth facility
Employees at Cornerstone Cottage alerted state officials to the dangers, only to be fired themselves Cornerstone Cottage opened in 2016 in Post Falls, Idaho, a booming bedroom community 25 miles

Wildfires can impact your mental health
Wildfires can be frightening and result in overflowing emotions. Fear, anxiety and even depression can arise before, during and after these natural disasters, but specialists say there are still resources to cope with the trauma that environmental emergencies can cause.
















