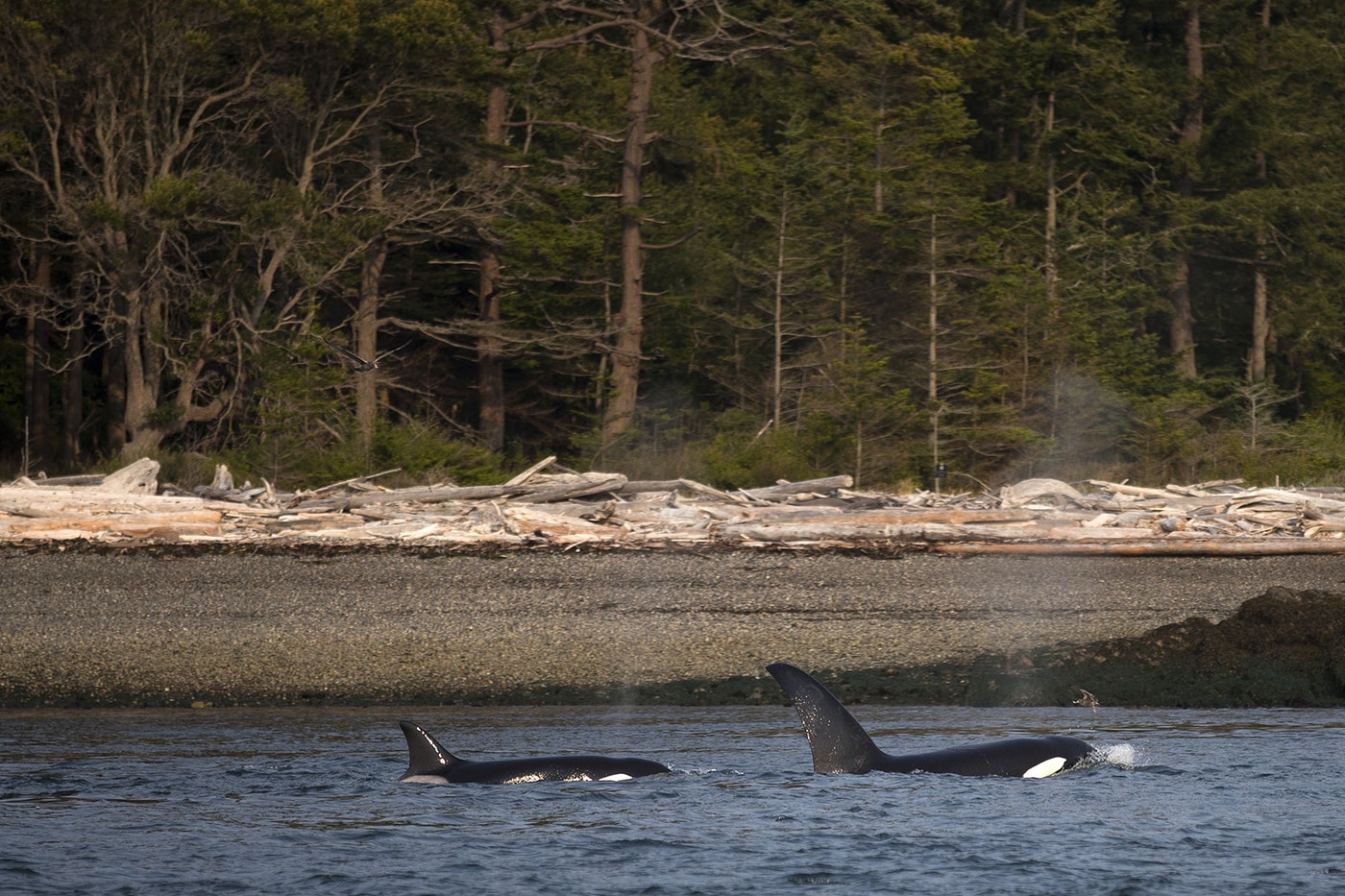Super Bacteria In Puget Sound Wildlife Could Endanger Humans
Read On
BY JOHN RYAN / KUOW
A leafy little tunnel runs through the undergrowth along the Black River in the Seattle suburb of Renton: an otter trail.
It’s in hidey-holes like this that river otters leave detailed evidence of human misdeeds.
Just downstream, in the Duwamish River, droppings left by river otters reveal toxic PCBsand other industrial waste.
Here, in a woodsy city park where the Black River carries runoff from nearby subdivisions and business parks, otter droppings contain our antibiotics and the super-bacteria that they can generate.
Bacteria that resist antibiotic drugs are becoming more widespread in our environment.
Last year, researchers reported finding35 kinds of multi-drug-resistant bacteria in the exhaled breaths of killer whales off the San Juan Islands.
Wildlife biologist Michelle Wainstein, working with Seattle’s Woodland Park Zoo, has been combing riverbanks along the Black, Green and Duwamish Rivers to find the defecating and socializing spots known as otter latrines. (Before leaving evidence for science, otters often congregate and even do a bouncy little move with their back legs that researchers call a scat dance.)
“At all of the field sites down in these urban areas, we have found strains ofE. colithat are resistant to various antibiotics,” Wainstein said.
Bacteria in otter scat from the Black River otter latrine flourished despite exposure to ampicillin, gentamicin, tetracycline, minocycline and sulfaoxazole, according to Wainstein’s preliminary findings.
Discarded or overused antibiotics can help disease-causing bacteria evolve new defenses.
Sewage treatment plants are usually effective at getting rid of bacteria — that’s their main purpose — but they fail to screen antibiotics and other pharmaceuticals from reaching otters or other aquatic organisms.
“Our waste ends up going somewhere,” Wainstein said. “And so they get exposed to our antibiotics.”
About a third of all antibiotics prescribed to humans are unnecessary or prescribed incorrectly, according to the Centers for Disease Control and Prevention.
Antibiotics are heavily used in livestock, too, often to promote growth, not treat disease. About 70 percent of medically important antibiotics are sold for use on livestock, according to the nonprofit Consumers Union.
A Washington Department of Fish and Wildlife report found Virginiamycin-M1, an antibiotic widely used on livestock, in native bay mussels at all 18 sites around Puget Sound where the researchers had submerged cages of the mussels as living pollution meters.
“They’re little sentinels,” Washington Department of Fish and Wildlife biologist Jennifer Lanksbury said of the filter-feeding mussels. “A canary in a cage.”
Last year was the first to see a decrease in the use of antibiotics for livestock, according to the U.S. Food and Drug Administration. Consumer groups welcomed that news and credited chicken producers’ efforts to reduce the routine use of antibiotics.
Yet beef, pork and turkey producers use more than ten times the quantity of medically important antibiotics to produce a pound of meat that chicken producers do, according to Consumers Union.
The resistant bacteria probably don’t do any more harm to wildlife than regular bacteria would. It’s almost unheard of for wild animals to be treated with antibiotics, though scientists did attempt to do so last summer in an ultimately unsuccessful effort to save the life of an ailing young orca known as J-50.
The much bigger risk is that these super-bacteria could find their way back into humans or livestock, and our life-saving drugs wouldn’t work on them anymore.
“Then we have no way to combat them,” Wainstein said.
Each year in the United States, at least 2 million people get an antibiotic-resistant infection, and at least 23,000 people die, according to the Centers for Disease Control and Prevention.
“Anyone handling crab or fish, if you stick your finger, you could get exposed to a resistant strain,” said National Oceanic and Atmospheric Administration microbiologist Linda Rhodes, who has studied the microbes found in resident orcas’ exhaled breaths.
“Humans are definitely putting pathogens that we’ve selected for resistance in the environment,” she said.
“Bacteria itself could come from leaking septic systems or stormwater runoff from streets,” Lanksbury said. “Human waste, pet waste, farming practices.”
Whenever a heavy rainstorm overwhelms sewer systems, untreated, bacteria-laden sewage floods directly into local waterways.
Rhodes said efforts to replace impervious surfaces like pavement with more absorbent surfaces could help reduce bacterial pollution.
“If you can slow the water down, it can snag a lot of particulates, particularly bacteria,” she said.
Once detained in a patch of soil, pathogens that thrive in our bodies often have a hard time competing against the soil’s own microbes.
Other researchers are now trying to see if restoring underwater habitats like eelgrass beds might help stem the tide of bacterial pollution into Puget Sound.
Related Stories:

He Spent $50K On A Tag To Kill A Noted Kittitas Valley Elk. What’s The Real Cost Of Trophy Hunts?
Over at least two decades, Washington business owner Tod Reichert spent hundreds of thousands of dollars buying exclusive hunting licenses he used to kill more than 100 elk. His license for the Ellensburg hunt, a “governor’s tag” auctioned to fund elk-related conservation efforts by state wildlife managers, cost him $50,000.

Replacing Plastic: Can Bacteria Help Us Break The Habit?
If civilizations are remembered for what they leave behind, our time might be labeled the Plastic Age. Plastic can endure for centuries. It’s everywhere, even in our clothes, from polyester leisure suits to fleece jackets.
A Silicon Valley startup is trying to get the plastic out of clothing and put something else in: biopolymers.

Timeline: A History Of Grizzly Bear Recovery In The Lower 48 States
At their peak, grizzly bears numbered more than 50,000 in the Lower 48. Facing threats from habitat loss, hunting and conflicts with people and livestock, their numbers dwindled to fewer than 1,000 in the lower 48 by the time the Endangered Species Act was implemented in 1975. Here’s a timeline of the management actions, court cases and notable events that have shaped grizzly bear recovery since their ESA listing through today.